This is a case report involving a novel setting of sonographic scan for thickness of superficial abdominal fat and a non-invasive approach for reduction of the fat thickness. A 38-year-old woman complained of her abdominal contour asymmetry after the laser-assisted liposuction performed two years ago. Compression-free sonographic scanning confirmed that her superficial abdominal fat was thicker in left side than that of right side. After 9 sessions of 40KHz therapeutic ultrasound, the contour asymmetry was reduced.
As human bodies age, local abdominal fat could increase gradually. The abdominal fat is anatomically categorized as visceral and subcutaneous (deep and superficial); the deep fat is associated with increased metabolic and cardiovascular risks (Kuk et al., 2006). For overweight individuals, the most common prescription for the fat reduction is calorie restriction and increased physical activities (Thomas et al., 2000). Some obese people may require medications and gastric surgeries depending on their response to the lifestyle interventions. But individuals who are not overweight, some complained of exercises being ineffective for the reduction of abdominal fat (Vispute et al., 2011). As a result, invasive laser assisted liposuction has been invented to reduce the superficial fat thickness (Goldman, 2006); non-invasive approaches such as therapeutic ultrasound (TU) has been used for the same purpose with preliminary evidence (Garcia and Schafer, 2013). However, no study has been done to observe if a non-obese subject’s one side abdominal area receives TU while the contralateral side serves as a control.
This case report was based on one non-obese female. Her age was 38, bodyweight was 55.4 kg and height was 150 cm. She complained of her abdominal contour asymmetry at umbilical level after the laser-assisted liposuction performed two years ago, she had not noticed the pre-operative asymmetry. The contour asymmetry is a common adverse event of the liposuction (Dixit and Wagh, 2013). Except the complaint, she was physically and mentally sound.
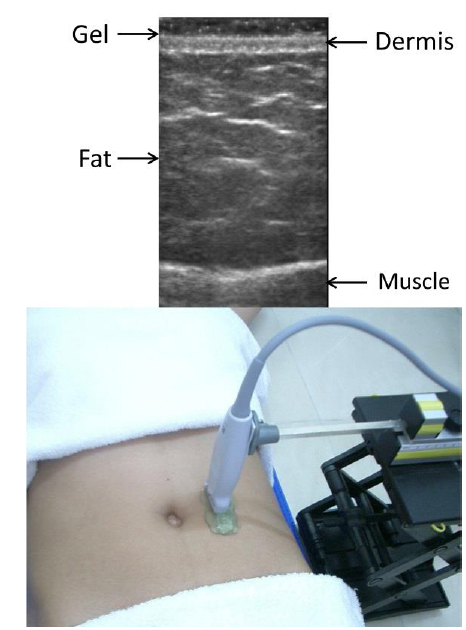
In order to quantify the contour asymmetry, a novel setting of sonographic scan for superficial abdominal fat was prepared in which B-mode ultrasound transducer (NanoMaxx, SonoSite Inc., USA) was held statically 4 cm lateral to umbilicus and floated at the top of abdominal skin (Fig. 1), thus the weight of the transducer would not deform the fat and affect the accuracy of the thickness measurement. The measurement showed that the subject's left side (affected side) was 48mm and the right side was 37 mm. Since the subject preferred the non-invasive approach for her asymmetry issue, she agreed to receive 40KHz TU for reducing the fat thickness of her left abdomen while the right abdomen (control side) needed no treatment; the sound wave was delivered at pulsed mode (300ms on: 300ms off) and the average intensity of 1W/cm2 for 15 minutes in each treatment (KUL-40, King Ultrasonic, Taiwan), a total of 9 treatments which were evenly distributed three times a week for 3 weeks.
After 3-weeks treatment, the subject was scanned using the above sonographic measurement (Fig. 1) that showed that the left side (affected side) was 41 mm (-14.6% thickness as 7 mm out of 48 mm), while the right side (control side) was 35 mm (-5.4% thickness as 2 mm out of 37 mm). In our department, the sonographic measurement had fair intra-rater repeatability as the test-retest difference was fewer than 5% at two-weeks interval based on the data of 12 non-obese adult females, thus, the reduction of fat thickness after the treatments was regarded substantial.
Bani et al. (2013) observed microscopic changes of the abdominal fat invasively suctioned from three obese subjects whose right abdomen pre-treated with TU and the left side without TU, they found that the adipocytes treated with TU were significantly smaller in size which signifies the triglyceride leakage. The present case report was based on a non-obese person who had complaint of her abdominal fat thickness asymmetry after liposuction; the asymmetry was reduced after the TU and the reduction was confirmed using B-mode ultrasound. Basically, the finding of the above two studies are rather parallel as the TU produced a lowering effect on the abdominal superficial fat.
While the present report suggested that the 40 KHz ultrasound could be used to minimize the abdominal contour asymmetry after liposuction, it still needs to be further confirmed in a study with adequate sample size.
Effects of therapeutic ultrasound for contour asymmetry