Traditional Korea medicine originated in ~3000 B.C. Since then, experience with remedies has accumulated to the point where Korean medicine has the academic knowledge to preserve human health [1]. Korean medicine is composed traditionally of herbal medicine and acupuncture. Herbal medicine has been used for thousands of years, is based upon the medicinal properties of plants, animals, and mineral products, and predates written human history. The clinical efficacy of herbal medicine is well recognized, and it is used by Korean medical practitioners [2]. Acupuncture refers to the stimulation of certain points on the body. It is one of the oldest healing practices in East Asia. Although Korean acupuncture has maintained a close relationship with traditional Chinese medicine, it has developed and sustained several unique aspects.
Pharmacopuncture is the combination of pharmacology and acupuncture. It is useful for the treatment or prevention of several diseases. Specifically, it reduces the side effects of drugs, and the excessive use of animal products, and the treatment costs in large animals [3]. Even though pharmacology and acupuncture are effective therapies in disease prevention and herbal treatment, the combination therapy is more efficient than either therapy alone. Because pharmacopuncture does not involve passage through the digestive system, the injection of subclinical doses of drugs into acupoints can result in more rapid effects than oral administration [4].
Sumsu (
The main components of sumsu are bufadienolides, including bufalin, cinobufotalin, resibufogenin and cinobufagin [15]. Bufadienolides are Na+/K+-ATPase inhibitors that can activate Na+/Ca2+ exchange in cardiac myocytes, increase intracellular calcium ions, and consequently increase the cardiac contractile force [16]. Bufadienolides also exert anti-tumor effects [17]. Bufalin can inhibit proliferation and induce differentiation and apoptosis in some cancer cell lines, including the U973, LNCaP, PC-3, THP-1, HL-60, and BEL-7402 cell lines [18-21]. Apoptotic effects of sumsu were observed
However, the potential antidepressant-like effects of sumsu pharmacopuncture have not yet been investigated. A recent study identified that sumsu contained serotonin and several bufadienolides [23]. Serotonin is a monoamine neurotransmitter. Alterations in serotonin neurotransmission have been implicated in the pathophysiology of severe depression [24]. The serotonin system plays a key role in the pathophysiology of major depressive disorders, and impaired serotonin function can lead to clinical depression [25, 26]. Therefore, we hypothesized that sumsu pharmacopuncture may attenuate the depression-like behavior induced by immobility stress.
In this study, we evaluated the antidepressant-like effects of sumsu pharmacopuncture in a model of chronic immobilization stress (CIS). CIS causes abnormal emotions and behaviors such as depression and anxiety [27]. Therefore, we examined the anti-anxiety and antidepressant-like effects of sumsu pharmacopuncture in a CIS mouse model. Three acupoints were used in this study: HT7, SP6, and GV20. HT7 is located at the depression on the posterior lateral side of the wrist, between the flexor carpi ulnaris and flexor digitorum superficialis tendons. SP6 is located at the proximal endpoint of the distal one fifth of the imaginary line connecting SP9 and the medial malleolus of the tibiofibula. GV20 is located at the vertex on the dorsal midline [28]. This study investigated the antidepressant-like effects of sumsu pharmacopuncture in mice by using an open-field test (OFT) and a forced-swim test (FST).
Sumsu (
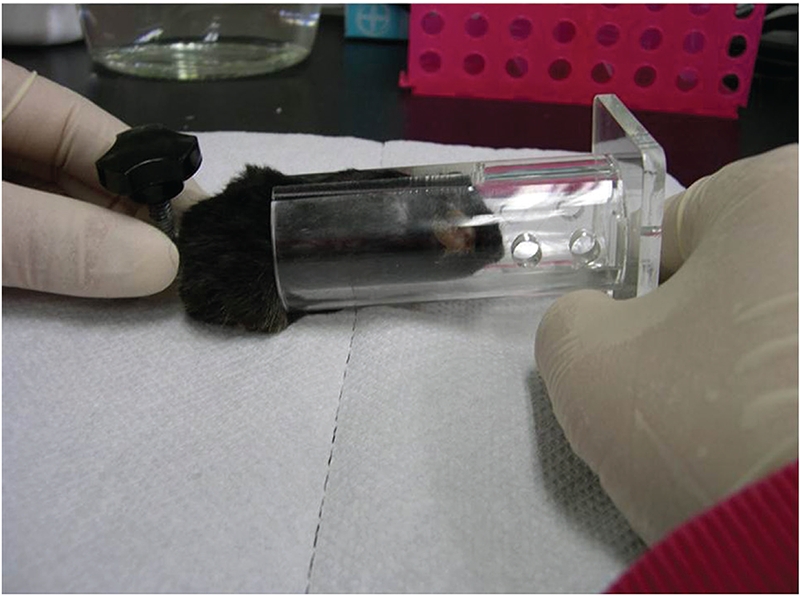
Chronic immobilization stress was induced in the animals; each group contained eight animals. The experimental schedule is shown in (Fig 1) Briefly, mice were adapted for 1 week; then the sham and the experimental groups were exposed to chronic restraining once a day in a restrainer for 2 hours from 14:00 - 16:00. Each mouse was placed in a 2 cm × 2 cm × 10 cm restrainer, which restricted their movement completely. The normal control group was not exposed to stress. After restraint, the sham group was injected with 20 μL of saline at each acupoint whereas the experimental group was treated with 20 μL of sumsu pharmacopuncture. The behavioral tests were then performed. Mice were sacrificed by cervical dislocation on the last day of the experiment.
The OFT is a commonly used measure of general locomotor activity and anxiety in rodents. Briefly, the apparatus is a brightly lit white Plexiglas box 50 cm × 50 cm × 50 cm, with its floor divided into nine squares. Squares adjacent to the walls formed the peripheral zone whereas the central area consisted of an inner square. Mice were placed in the central zone, and their movements were tracked using a video tracking system Smart (PanLab Harvard Apparatus, Holliston, Massachusetts, USA) for 5 minutes. The distance traveled and the time spent in the central vs. the peripheral zones of the open field were calculated.
The FST was performed according to the commonly-used procedure. The FST apparatus consisted of a transparent Plexiglas cylinder (35-cm height, 20-cm diameter) filled to a 20-cm depth with water at room temperature. Mice were placed in a cylinder of water at 23 - 25°C. The duration of immobility during the last 4 minutes of a 6-minute test was scored. Mobility was defined as any movement beyond that necessary to maintain the head above water. At the end of the test, mice were removed from the water, dried with a towel, and returned to their cages.
Statistical analyses were performed using statistical pakage for the social sciences (SPSS) ver. 18 (SPSS Inc.), and data were analyzed using the one-way analysis of variance (ANOVA). Scheff’s or Tukey’s post-hoc test were used to compare significant ANOVA results. Results are presented as means ± standard errors (SEMs). The level of significance was defined as
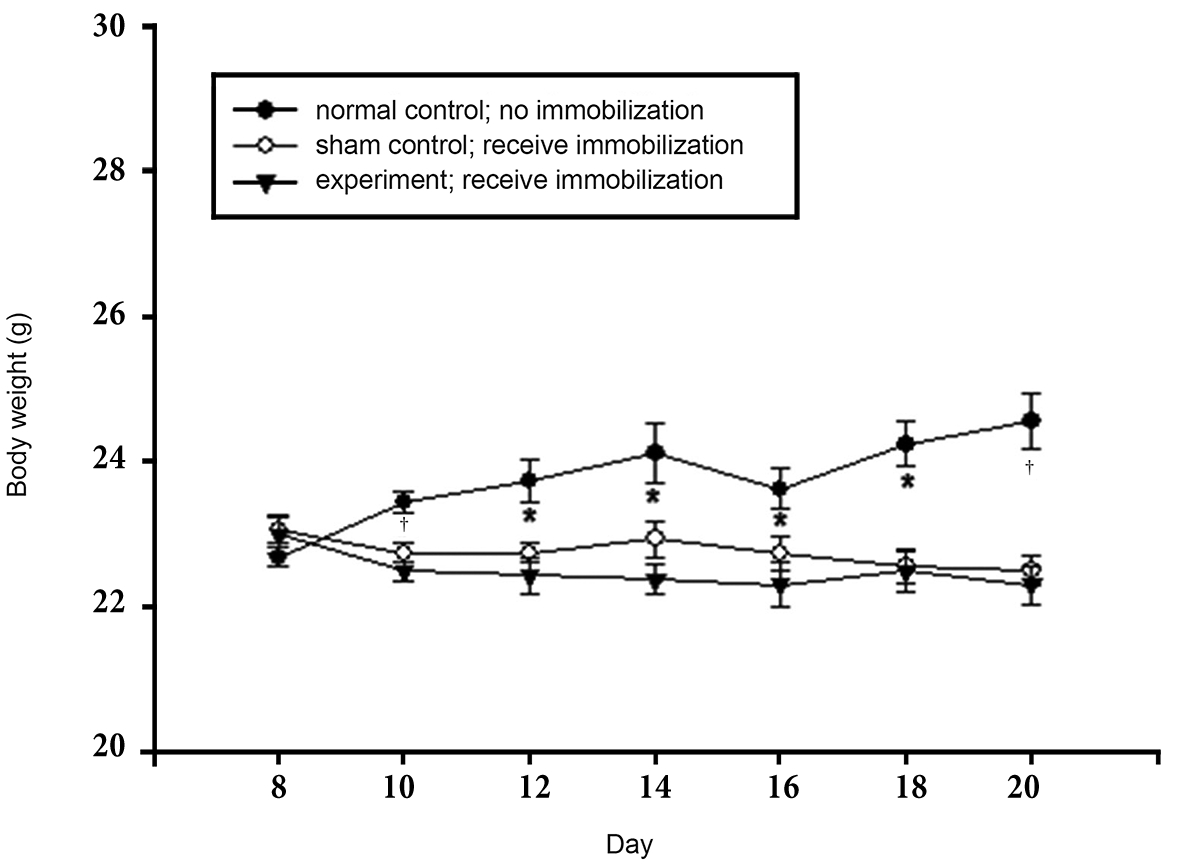
We used chronic restraint stress for 2 weeks using a restrainer (Fig 2) as the depression-like behavior model. Stress had a significant effect on body weight over the duration of the stress exposure period. Weight was measured during this period every other day (Fig 3). The sham and the experimental groups were subjected to immobilization stress for 2 weeks, but did not gain weight; in contrast, the normal control group gained significant body weight (
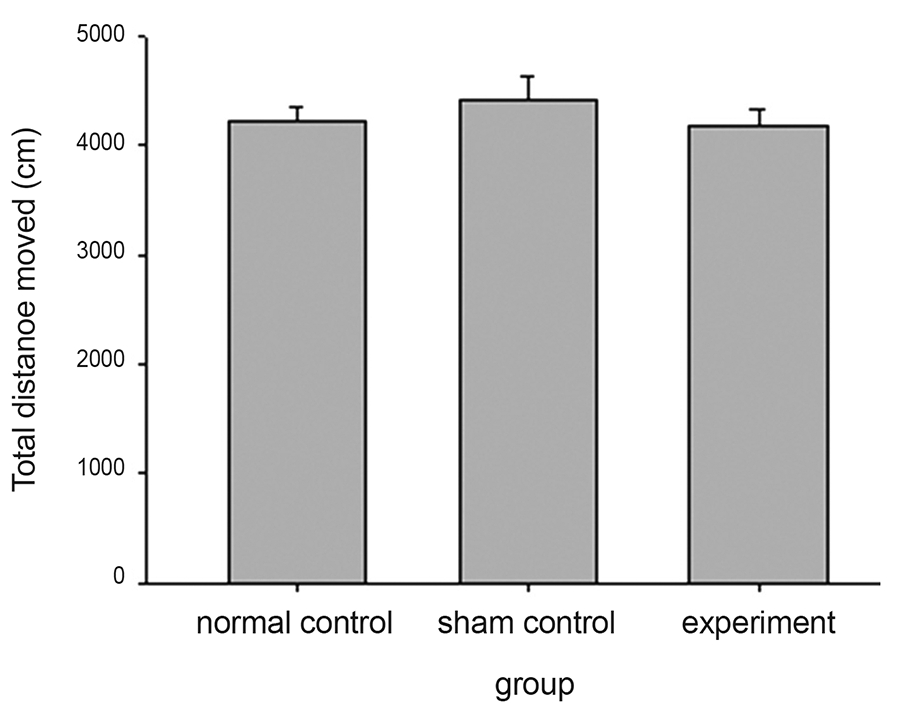
We next assessed the ambulatory movement of the pharmacopuncture- treated mice by using an OFT. We evaluated the total distance traveled using a video tracking system Smart (PanLab Harvard Apparatus, Holliston, Massachusetts, USA) for 5 minutes. As shown in (Fig 4), there were no significant differences between groups (
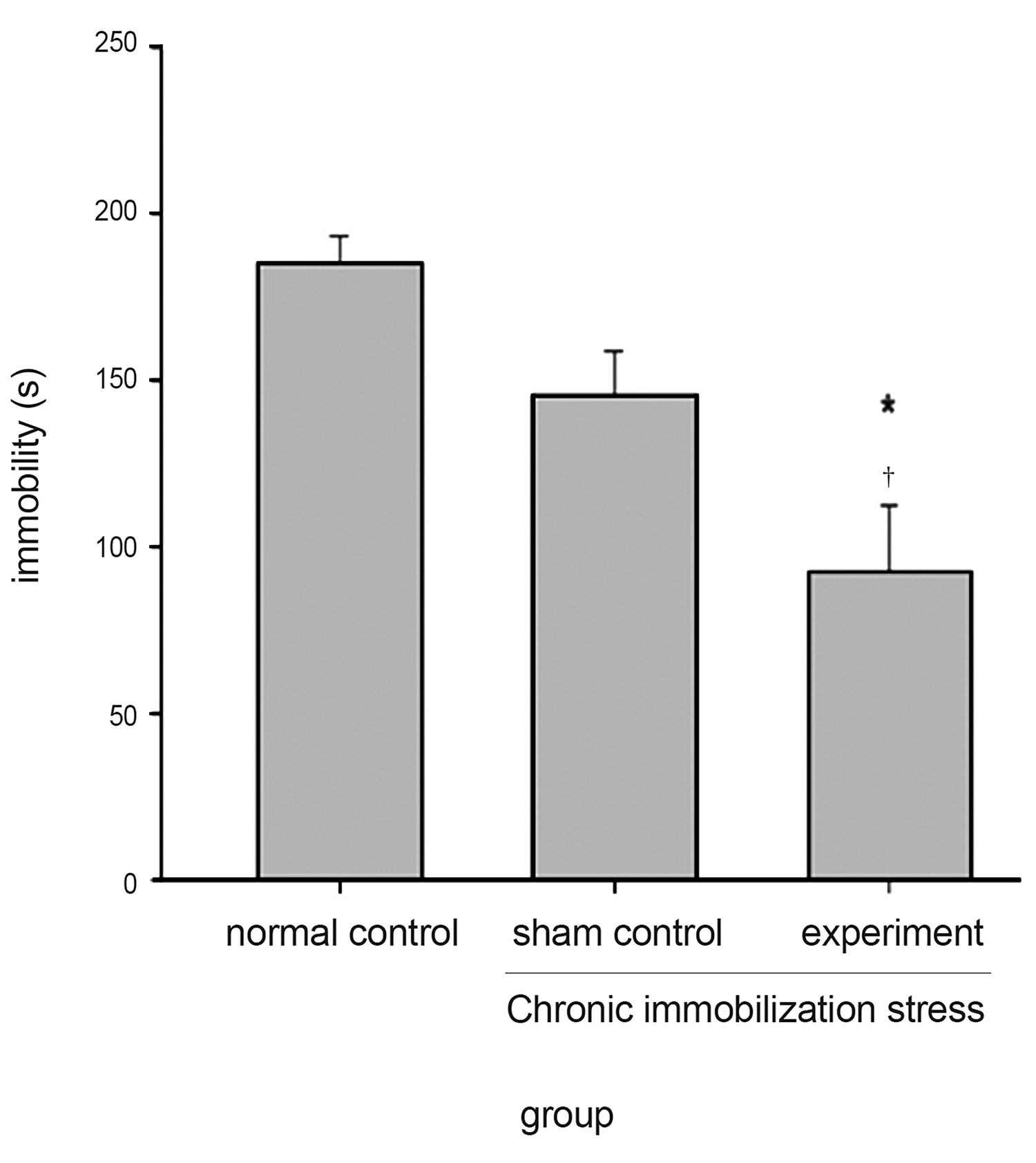
Next, we investigated the antidepressant-like effects of sumsu pharmacopuncture by using the FST. Sumsu pharmacopuncture significantly reduced the immobile time in the FST (
Depression is a major chronic disease and a common affliction that will affect ~ 15% of individuals in their lifetimes [29]. The World Health Organization (WHO) predicted that it would be the second most common disease by 2020 [30]. The therapeutic agents currently available for treating depression are successful in ~ 65% - 70% of patients, but serious side effects may limit these treatment strategies [31]. Therefore, we evaluated the efficacy of treatment of depression by using the traditional methods of sumsu pharmacopuncture. Acupuncture has long been used to treat diseases. However, the way in which pharmacopuncture stimulation in experimental animals modulates depression or anxiety is unknown. Acupuncture stimulation of Baihui (GV20) has been reported to be able to relieve some conditions such as headaches, anxiety, and dizziness [32-34]. More recently, pharmacopuncture and herbal acupuncture (an integration of acupuncture and herbal therapies) were introduced to optimize the benefits of acupuncture and herbal medicine by injecting minute quantities of herbs, medicines, blood, oxygen, and allergens [35] into acupoints. However, few reports describe the use of sumsu pharmacopuncture as an antidepressant. One of the main ingredients in sumsu is serotonin (5-hydroxytryptamine [5-HT]), which is associated with mood, appetite, and sleep, as well as with cognitive functions such as memory and learning. The modulation of serotonin at synapses is thought to be a major mechanism of action in several classes of pharmacological antidepressants. Herbal medicines, for example, St John’s wort, may be effective alternatives for treatment of depression [36]. Therefore, the aim of this study was to evaluate the antidepressant- like effects of sumsu pharmacopuncture in mice.
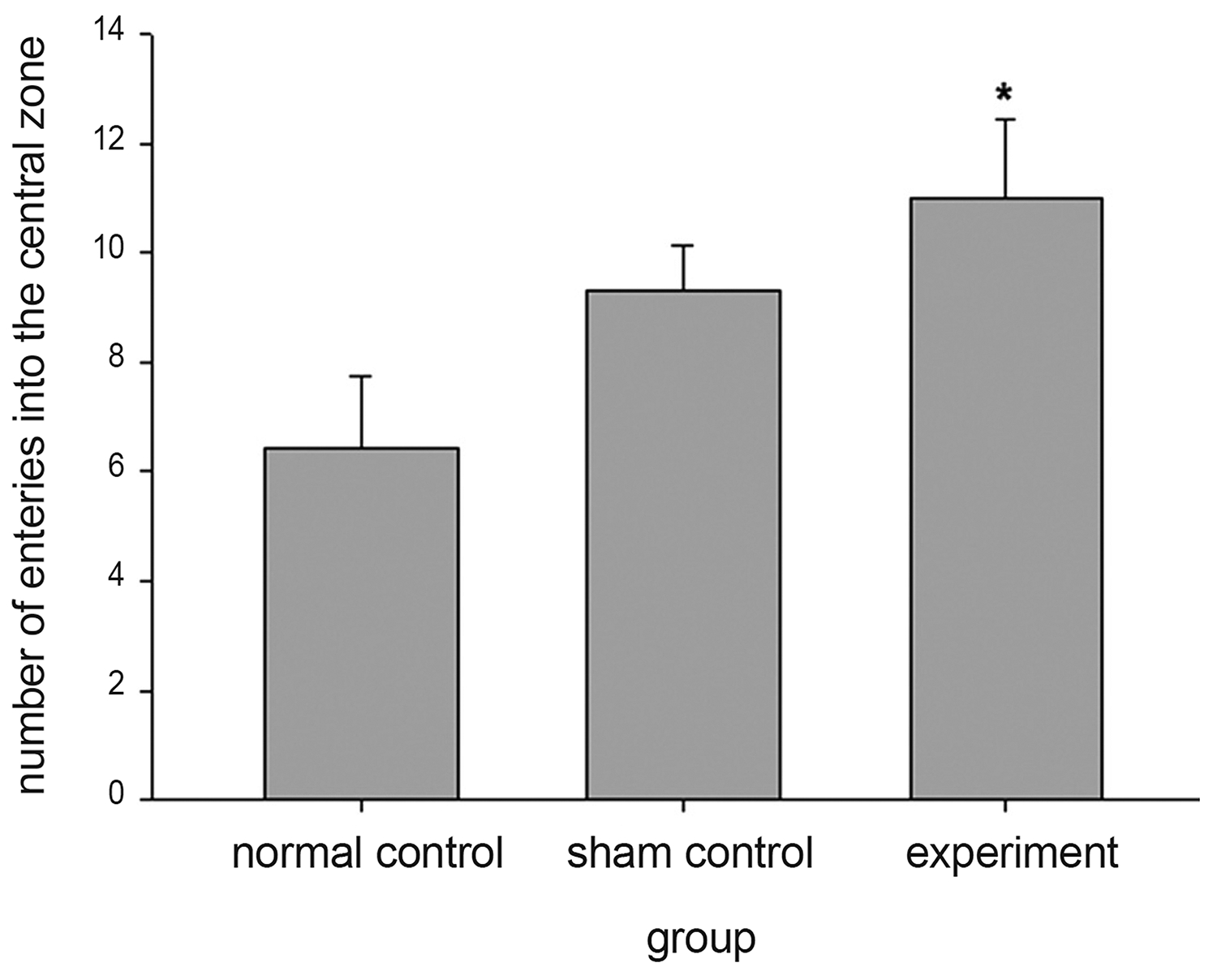
We used behavioral CIS animal models with the OFT and the FST. CIS induces repeated transient elevation of plasma corticosterone [37] and reduces glucocorticoid receptor expression. Furthermore, chronic mild stress induces depressant- like behavioral changes, such as working memory and learning deficits [38-40]. Therefore, the CIS model is appropriate for studies of depression. In the present study, we demonstrated that sumsu pharmacopuncture exerted antidepressant- and anti-anxiety-like effects in the OFT and the FST. The OFT is one of the most commonly used tests in animal psychology [41]. Anxiety behavior in the open field is elicited by two factors: individual testing (the animal is separated from its social group) and agoraphobia (the arena is very large relative to the animal’s breeding or natural environment). An increase in central locomotion, or in time spent in the central part of the device, without modification of total locomotion and vertical exploration can be inferred as an anxiolytic-like effect; conversely, the reverse behavior, is associated with anxiogenic effects [42]. In this study, there were no changes in total locomotion, but the number of entries into the central zone, particularly in the sumsu-pharmacopuncture-treatment group, was increased.
The FST is used to measure the effects of antidepressant drugs. We evaluated the effects of sumsu pharmacopuncture on changes in the immobility time in an inescapable acrylic glass cylinder filled with water based on escape behavior and active swimming. This immobility time is commonly decreased by antidepressants. Therefore, the FST can assess the behavioral state associated with depression- like symptoms [43-45]. The FST results showed that the immobility time in the group treated with sumsu pharmacopuncture was decreased compared to the immobility times in the other groups. The OFT allowed us to determine whether the behavioral deficits were affected by locomotor activity; there were no significant differences in total movement among the groups. However, the FST demonstrated significantly decreased immobility, suggesting that sumsu pharmacopuncture treatment exerted antidepressant-like effects.
Sumsu pharmacopuncture is not yet being widely used in clinics. However, our results suggest that it may be an effective antidepressant agent. However, we did not investigate its mechanism of action; therefore, additional studies are needed to determine which constituents contribute to the antidepressant-like effects of sumsu pharmacopuncture. Additional animal behavioral studies (such as the tail-suspension test and the elevated plus maze test) are needed to demonstrate that the antidepressant-like effects of sumsu pharmacopuncture can be sustained in the long term.
The results demonstrate that sumsu pharmacopuncture exerts antidepressant-like and anti-anxiety-like effects. Therefore, sumsu pharmacopuncture has therapeutic potential for treating neuropsychiatric disorders, such as anxiety and depression.
![Experiment schedule. Animals were divided into three groups: normal control (n = 8), sham control (chronic immobilization stress
[CIS] + acupuncture; n = 8), and experimental (CIS + pharmacopuncture; n = 8). The normal control group was not restrained or exposed to acupuncture.
The sham control and the experiment groups were treated using a 100-μL syringe to inject 20 μL of saline or pharmacopuncture at the
acupoints HT7, SP6, and GV20. CIS, chronic immobilization stress; OFT, open-field test; FST, forced-swim test.](http://oak.go.kr/repository/journal/13086/DHOCBS_2014_v17n2_27_g001.jpg)