The brain normally receives cerebral blood flow in the amount of 50 ml/100 g/min [1]. When the amount of cerebral blood flow drops under 10 ml/100 g/min, it results in energy metabolism disorders such as intracellular acidosis, often leading to fatal ischemic cranial nerve tissue impairment [2, 3]. In addition, when the decreased flow lasts longer than 5 min, brain function disorder or brain tissue impairment irreversibly occurs and results in various symptoms, including disturbance of consciousness, speech disorder, and motor disorder [4, 5]. A few studies on the effects of pharmacopuncture on cerebral hemodynamics exist. Cervi pantotrichum cornu pharmacopuncture at BL23 and BL52 increased the regional cerebral blood flow (rCBF) while it decreased the mean arterial blood pressure (MABP) [6]. Carthami flos pharmacopuncture at GV15 showed an anti-ischemic effect through an improvement of cerebral hemodynamics in transient cerebral ischemia [7].
Male rats in the Sprague, Dawley family with weights of approximately 250 g (Samtaco, Korea) were purchased as subject animals and were used for the experiments. The animals were used after having been stabilized for more than 5 days in a breeding environment (interior temperature 24℃, humidity 55 ± 5%, and 12-h dark/light cycle). The BUM pharmacopuncture solution was prepared in the aseptic room of the Korean Pharmacopuncture Institute [11]. BUM, 1 ul, 5 ul, 25 ul, and 125 ul, was administrated to Fengfu (GV16) by using an insulin syringe (ultrafine 2, BD, U.S.A.), following dilution to 1 ml. Fengfu (GV16) was taken between the external occipital protuberance and the atlas on the posterior midline of the head. The rats were anesthetized with 750 mg/kg of urethane (Sigma, U.S.A.) by using peritoneal injections. Then, the parietal bone was exposed by dissecting the scalp along the center line. At a point 4-6 mm to the side and 0.2-1 mm to the front of the bregma, the operation for a 5- to 6-mm skull window was conducted. The needle probes for the laser Doppler flow meter (Transonic Instrument, U.S.A.) were carefully inserted toward the cerebral pial artery and were carefully kept perpendicular to the parietal cortical surface. After having been stable for certain periods of time, the rCBF was monitored for BUM injected into Fengfu (GV16), the concentrations of which was increased by 5 times in 30-min intervals. To measure the MABP, we fixed the anesthetized rats on heat pads to stabilize the body temperature at 37.5℃. A polyethylene tube was inserted in the aorta femoralis of the rat, and the data were transmitted to the data acquisition system (Maclab, U.S.A.) through a pressure transducer (Grass, U.S.A.). The MABP was measured with BUM in the same manner as the rCBF was measured. Methylene blue (0.01 mg/kg, intraperitoneal, MTB, Sigma), a inhibitor of guanylate cyclase, and indomethacin (1 mg/kg, intraperitoneal, IDN, Sigma), a inhibitor of cyclooxygenase, were used to pre-treat normal rats, and the rCBF and the MABP were observed following the injection of 25 ul of BUM. For cerebral ischemia induction, the middle cerebral artery (MCA) closing method according to Longa et al. was used [12]. Thirty min after the MCA fundus had been closed, a 1-ml saline solution containing 25-ul BUM was injected. One hundred twenty min after the closing, the blood flow was reperfused, and the change in the rCBF was monitored for 240 min.
The data for the rCBF and the MABP were analyzed by using the SAS program (ver. 9.2). The statistical significance was determined using the repeated measure ANOVA.
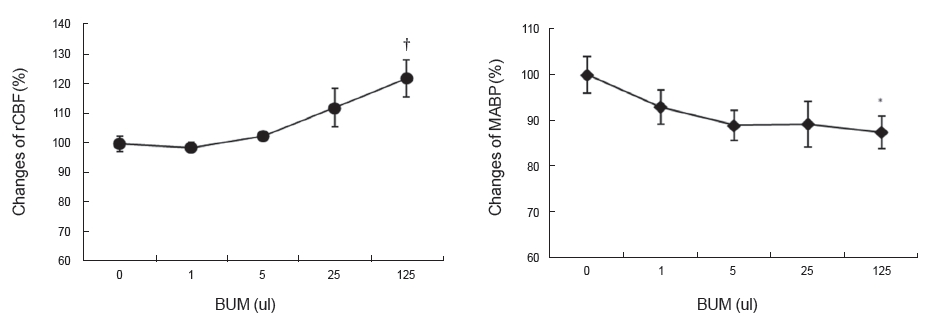
Compared to the rCBF of normal rats without BUM (100 ± 18%), the rCBFs were 98.74 ± 0.02%, 102.58 ± 0.64%, 112.14 ± 0.28%, and 122.08 ± 0.71% with 1 ul, 5 ul, 25 ul, and 125 ul of BUM, respectively, indicating significant increases in a dose-dependent manner (P = 0.003; (Fig 1)A). On the other hand, the MABP decreased to 93.00 ± 0.67%, 88.94 ± 0.32%, 89.14 ± 0.26%, and 87.38 ± 0.97% with 1 ul, 5 ul, 25 ul, and 125 ul of BUM, respectively, compared to that without BUM, indicating significant decreases in the blood pressure in a dose-dependent manner (
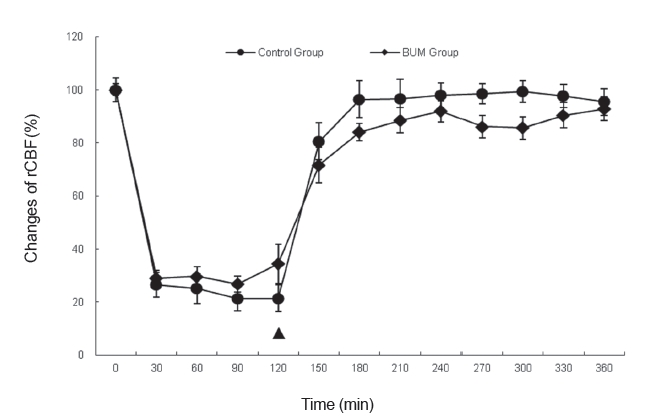
To observe BUM’s effect on the rCBF change in rats with induced cerebral ischemia, we observed the changes in the rCBF after reperfusion following the administration of BUM to the rats in which cerebral ischemia had been induced by using the MCA closing method. The rCBF results for the two groups showed significant differences in the group (F = 0.60, P = 0.452), the time (F = 138.48, P < 0.001) and the interaction according to the group and the time (F = 2.31, P = 0.036). Thus, the rCBF change was observed to be improved stably in the BUM-treated group compared to the control group in which the changes were unstable when going through the reperfusion in the cerebral ischemia state (Fig 4)
The rCBF is directly proportional to the blood pressure and the diameter of the blood vessel. The higher the blood pressure is, the more the rCBF is. The dilation of the blood vessel arises from relaxation of smooth muscles by secretion of prostaglandin, an endothelium-derived relaxing factor. Prostaglandin is an effective drug for the rennin and angiotensin system and acts to relax vessels and to lower the blood pressure. The blood pressure is controlled by the heart rate, the contraction of the myocardium, the peripheral blood vessel and the intrinsic active substances in the body [13, 14]. This study shows that the rCBF increases to a value significantly higher than the base value when BUM is administrated to normal rats. Considering that the cerebral blood flow is proportional to the mean blood pressure and the cerebrovascular diameter, this result suggests that BUM may dilate the brain’s blood vessels.
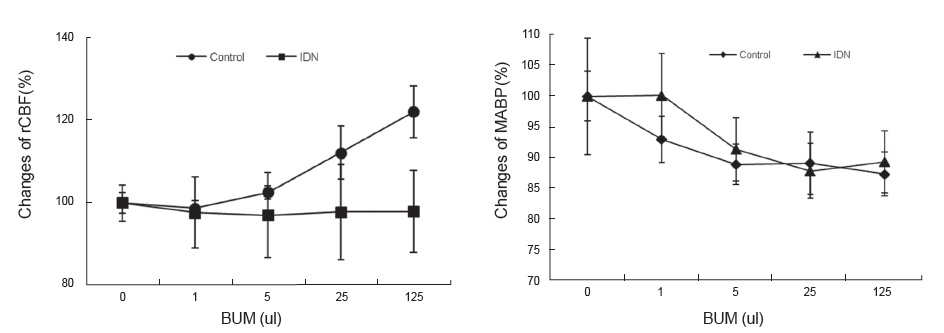
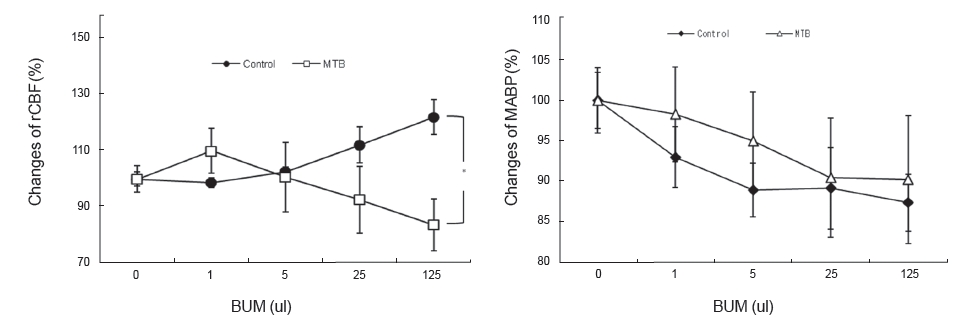
In this study, to verify what mechanism causes BUM to increase the rCBF significantly, we pretreated the rats with indomethacin [15], an inhibitor of cyclooxygenase involved in vessel dilation, and with methylene blue [16], an inhibitor of guanylate cyclase, and we observed the mechanism. Considering such results, according to the report by Shin et al. stating that the reduction of the rCBF by methylene-blue pretreatment was related to guanylate cyclase, an enzyme creating cyclic guanosine monophosphate [17-19], and reports by Bakalova [20] and Okamoto et al. [21] stating that the reduction of the rCBF with indomethacin treatment was related to cyclooxygenase, the significantly increased rCBF after BUM administration is considered to be the result of cerebrovascular dilation due to vitalized guanylate cyclase.
The ischemic brain impairment occurring due to the reduction of cerebral blood flow is more serious when the blood is re-supplied than when the cerebral blood flow is reduced [22-24]. The reperfusion of the ischemia area intensifies the neuron impairment by causing biochemical and cytogenic reactions in series and by causing impairments not only in the regionally relevant tissues, but also in other organs. This action is assumed to be related to non-specific toxins, vasoreactive materials, lactic acid and oxygen-free radicals. Therefore, the maintenance of the stable rCBF after reperfusion may become a critical index for treatments to prevent brain impairment [25]. In this study, the rCBF of the BUM group was significantly improved and became stable while the rCBF of the control group under a cerebral ischemia condition showed an unstably increasing state. The results may suggest that BUM controls the impairment of brain nerve cells caused by non-specific toxins, vasoreactive materials and oxygen-free radicals occurring due to cerebral ischemia, although whether the stimulation by needles per se, beside BUM injection, added any effects cannot be ruled out. In conclusion, when brain impairment occurs due to cerebral ischemia, BUM is shown to have an anti-ischemic effect by dilating the diameters of cerebrovascular vessels, which is related to guanylate cyclase, to provide a stable cerebral blood flow.
This study demonstrated that injection of BUM into Fengbu (GV16) increased the rCBF in a dose-dependent manner in the normal state; furthermore, it improved the stability of the rCBF in the ischemic state upon reperfusion. Also, the effects of BUM on the rCBF were attenuated by inhibition of guanylate cyclase, suggesting that the effects involved the guanylate-cyclase pathway.