Pharmacopuncture therapy is a new acupuncture therapy based on herbal medicine, acupuncture & moxibustion medicine, and meridian theory [1]. Through a single procedure, it can achieve both the effects of acupuncture and herbal medicine. As the pharmacopuncture does not pass through the digestive system, it works fast and it has effects that oral administration does not have [2]. Highly effective herbs are selected, depending on the disease. Pharmacopuncture fluid is extracted from these selected herbs and injected into the meridian points or sore spots [3].
The constituents of the Chukyu (spine-healing) pharmacopuncture are
Several studies on the relation between the toxicity and the composition of Chukyu pharmacopuncture have been conducted. Koo et al. conducted a philological study on the toxicity of
The current research trend for single-dose toxicity testing of extracts is to study acute and subacute toxicity through Good Laboratory Practice (GLP) regulations. All the experiments for this research were conducted at Biotoxtech, a non-clinical studies authorized institution, under the GLP. This study was performed to analyze the single-dose toxicity and the lethal dose of Chukyu pharmacopuncture in rats.
The Chukyu pharmacopuncture was prepared in a sterile room at the Korean Pharmacopuncture Institute (K-GMP). After the mixing process with pure water, the pH was controlled to between 7.0 and 7.5. NaCl was added to make a 0.9% isotonic solution. The completed extract was stored in a refrigerator (2.1-6.6℃).
The animals used in this study were 6-week-old Sprague-Dawley rats. The reason Sprague-Dawley rats were chosen is that they have been widely used in safety test in the field of medicine, so the results can be easily compared with many other data bases. The mean weights of the rats were 179.8-198.5 g and 143.8-173.1 g, respectively, for the male and the female rats at the time of injection. For all animals, a visual inspection was conducted; all animals were weighed using a CP3202S system (Sartorius, Germany). During 7 days of acclimatization, the general symptoms of the rats were observed once a day. The weights of the rats were recorded on the last day of acclimatization. No abnormalities were found.
The temperature of the lab was 20.0-22.8℃, and the humidity was 48.5-65.9%. Enough food (Teklad Certified Irradiated Global 18% Protein Rodent Diet 2918C) and UV-filtered water were provided.
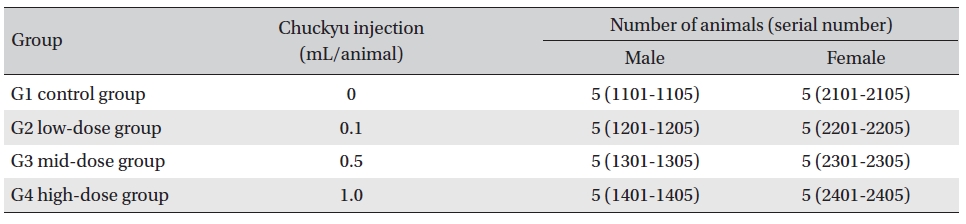
Groupings were done after 7 days of acclimatization. Animals were selected if their weights were close to the mean weight. In total, 20 male rats and 20 female rats were selected. The animals were randomly distributed into 4 groups (5 mice per group) as shown in, Table 1.
In clinical applications, the usual dose for Chukyu pharmacopuncture is 1.0 mL per treatment. No death occurred in the pilot test in which 1.0 mL of Chukyu pharmacopuncture was injected into each male and female rat. In this study 1.0 mL/animal was set as a high-dose, and 0.5 mL/ animal and 0.1 mL/animal were set as mid and low doses, respectively. In the control group, 1.0 mL of normal saline solution was administered. A single dose, 0.1 and 0.5 mL/ animal, was injected into the left thigh muscle of the rats in the low and mid-dose groups, respectively, and 0.5 mL of Chukyu pharmacopuncture was injected into each thigh muscles of the rats in the high-dose groups, for a total of 1.0 mL/animal, by disposable syringes. This study was conducted under the approval of the Institutional Animal Ethic Committee of Biotoxtech Co., Ltd..
From the 1st day to 14th day after treatment, the general symptoms were examined once a day. On the day of dosing (day 0), the general symptoms (side effects, revealing time, recovery time, etc.), as well as mortality, were examined at 30 minutes and at 1, 2, 3, and 4 hours after injection. The weights were measured immediately before treatment and at 3, 7 and 14 days after treatment. After fasting for more than 18 hours, the rats were anesthetized by using
The weight, hematologic examination and blood chemical test results from the experiments were analyzed by using SAS (Statistical Analysis System, version 9.2,9.3, SAS Institute Inc., USA). A Bartlett test was conducted to evaluate the homogeneity of the variance and the significance. The one-way ANOVA test was conducted when the homogeneity of the variance was recognized, and the Kruskal-Wallis test was conducted post-hoc.
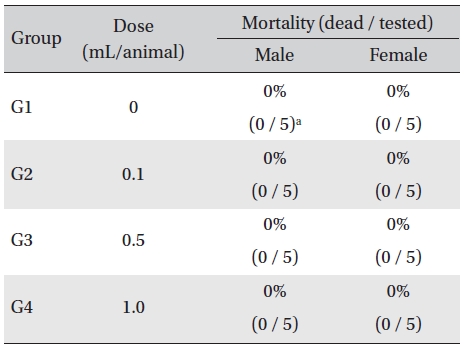
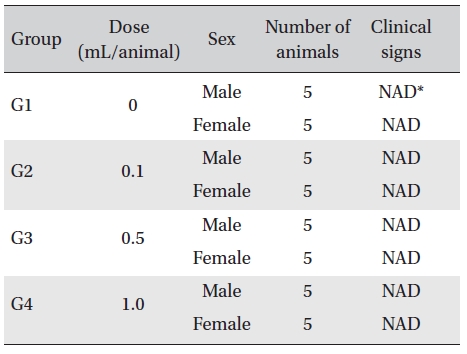
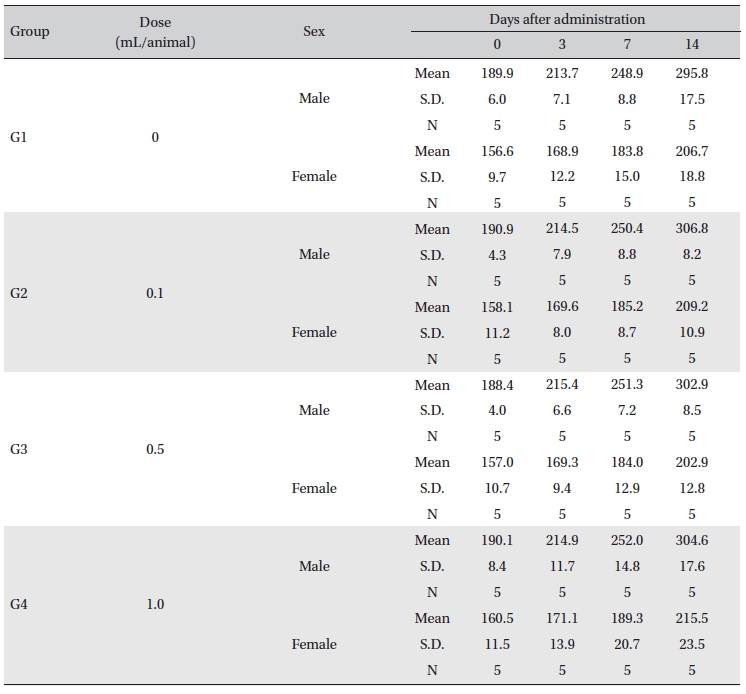
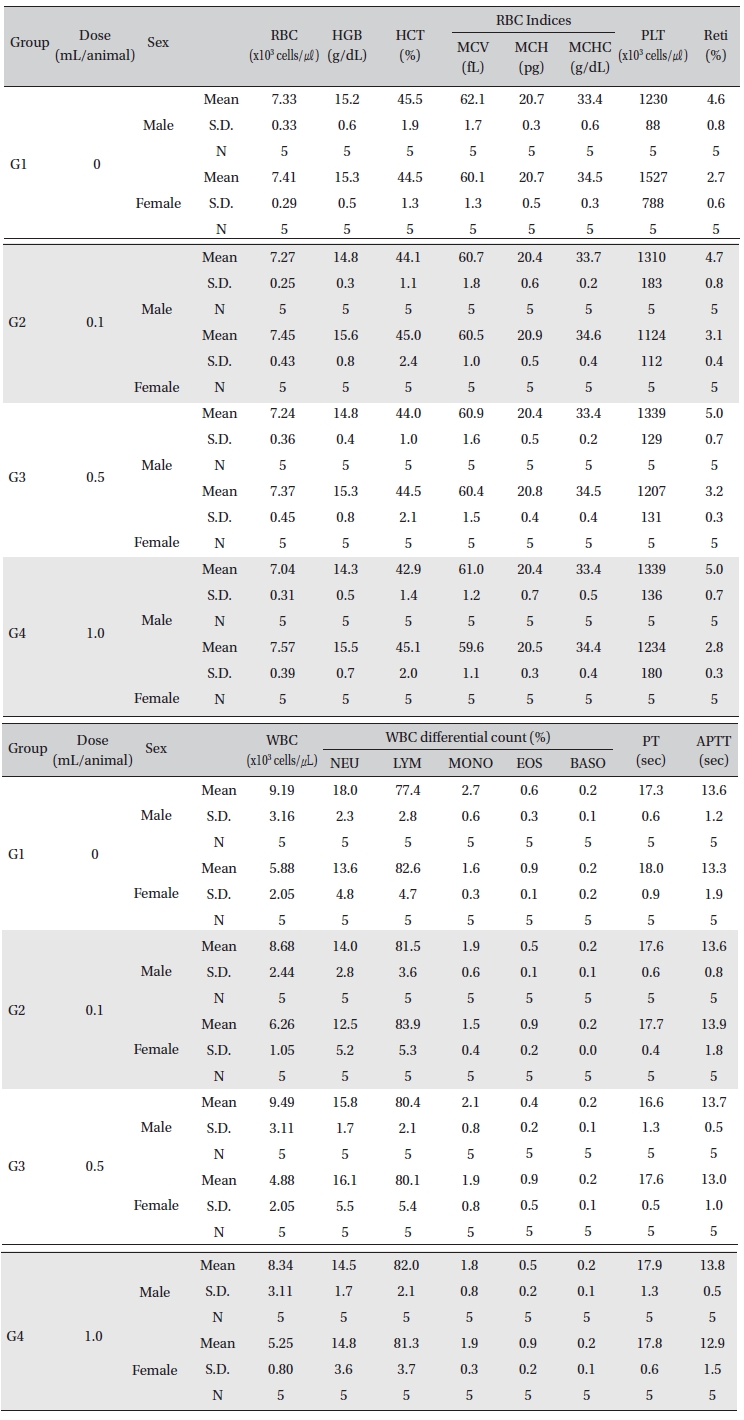
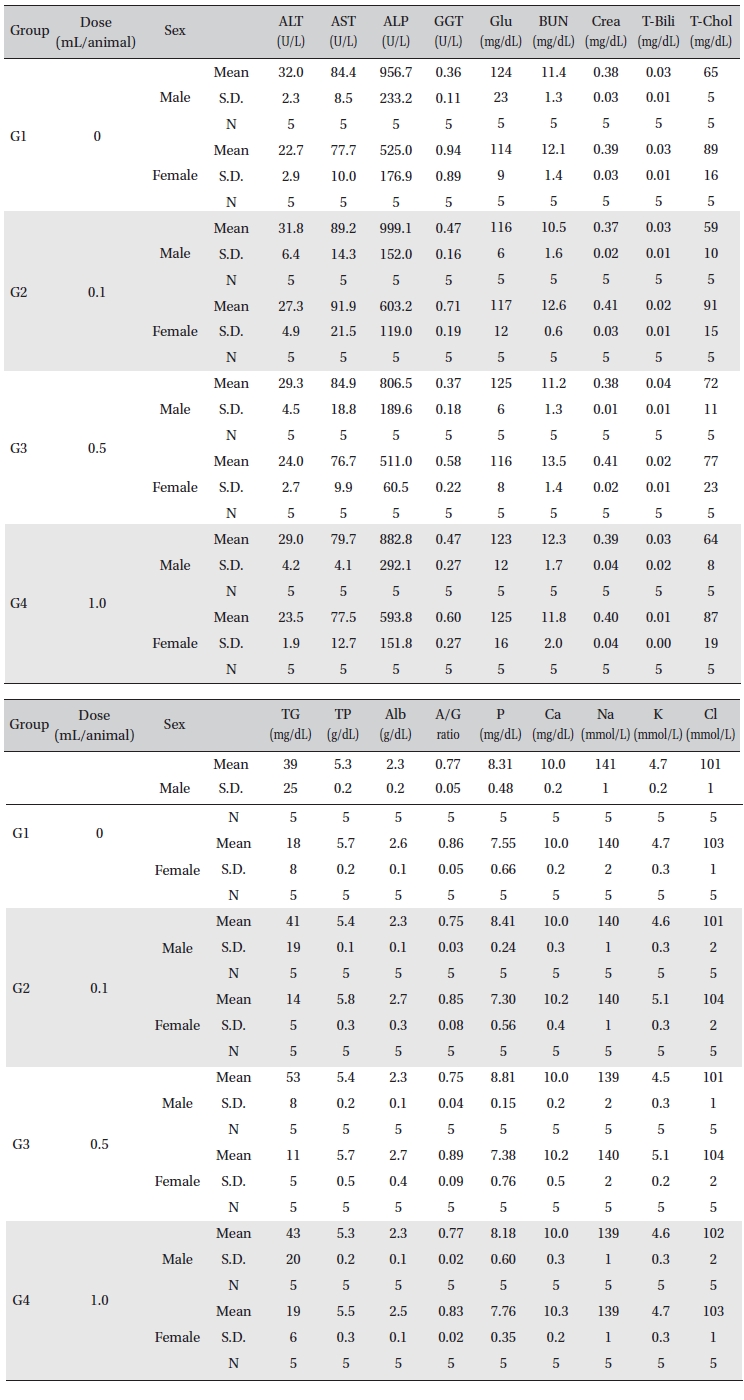
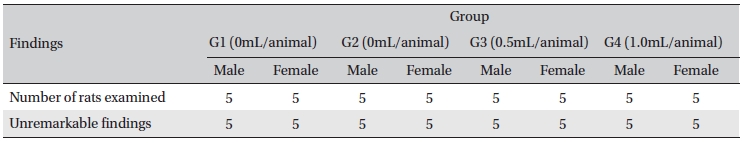
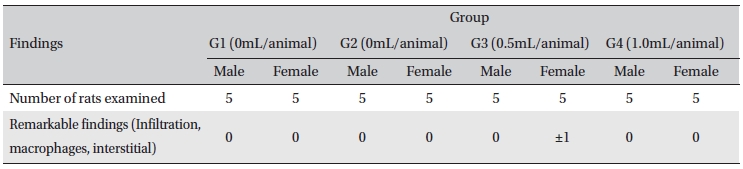
In this study, no deaths or abnormalities occurred in any of the groups (Table 2,3). In addition, no changes in weight were observed in any of the groups (Table 4). Finally, no meaningful changes in the hematological examination, blood chemical test or necropsy were noted (Tables 5, 6, 7). On histopathological examination, interstitial infiltrating macrophages were found in one female rat in the 0.5-mL/animal group, but no significant changes in the brain, lungs, liver, kidney and spinal cord related to the injections were found in the other groups (Table 8).
Chukyu pharmacopuncture is used widely in clinics. Until now, there has been only one clinical review on the effects of Chukyu pharmacopuncture [4]. On the other hand, there have been many studies on the component herbs of this pharmacopuncture.
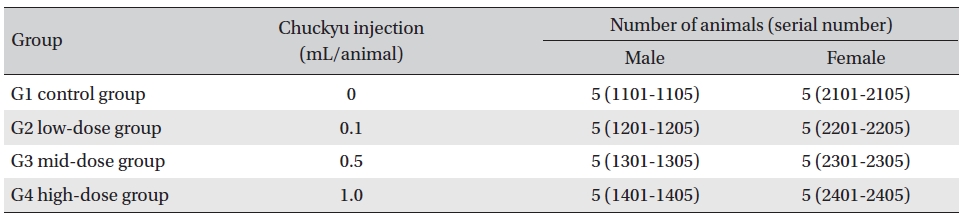
Groups of animals
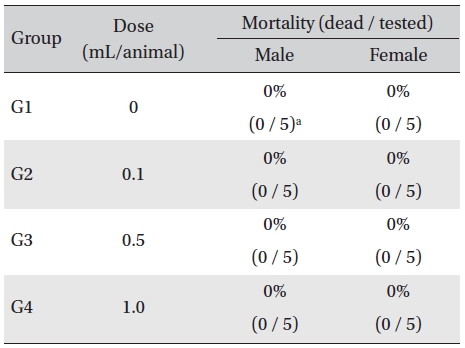
Mortality
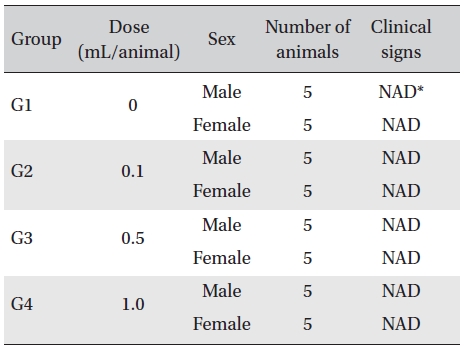
Clinical signs
[Table. 4] Body weights in grams
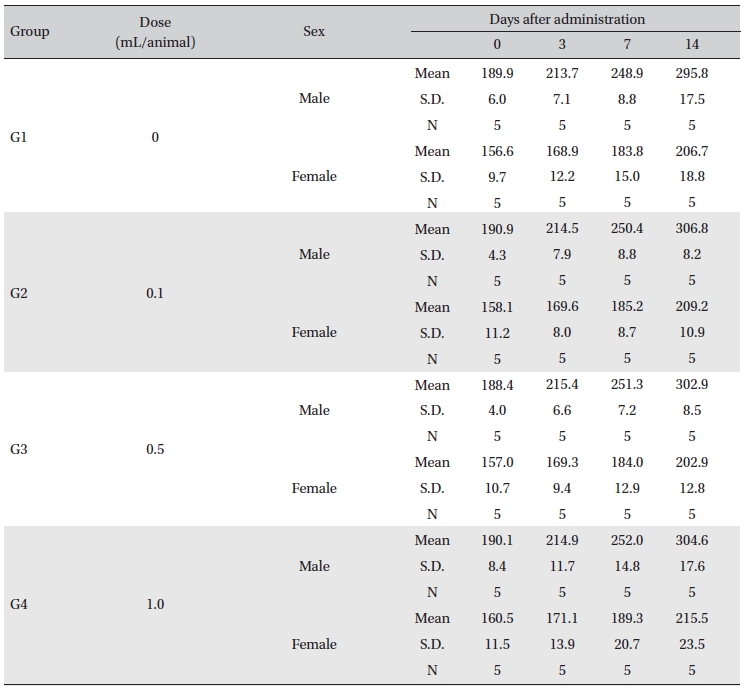
Body weights in grams
[Table. 5] Mean hematology parameters
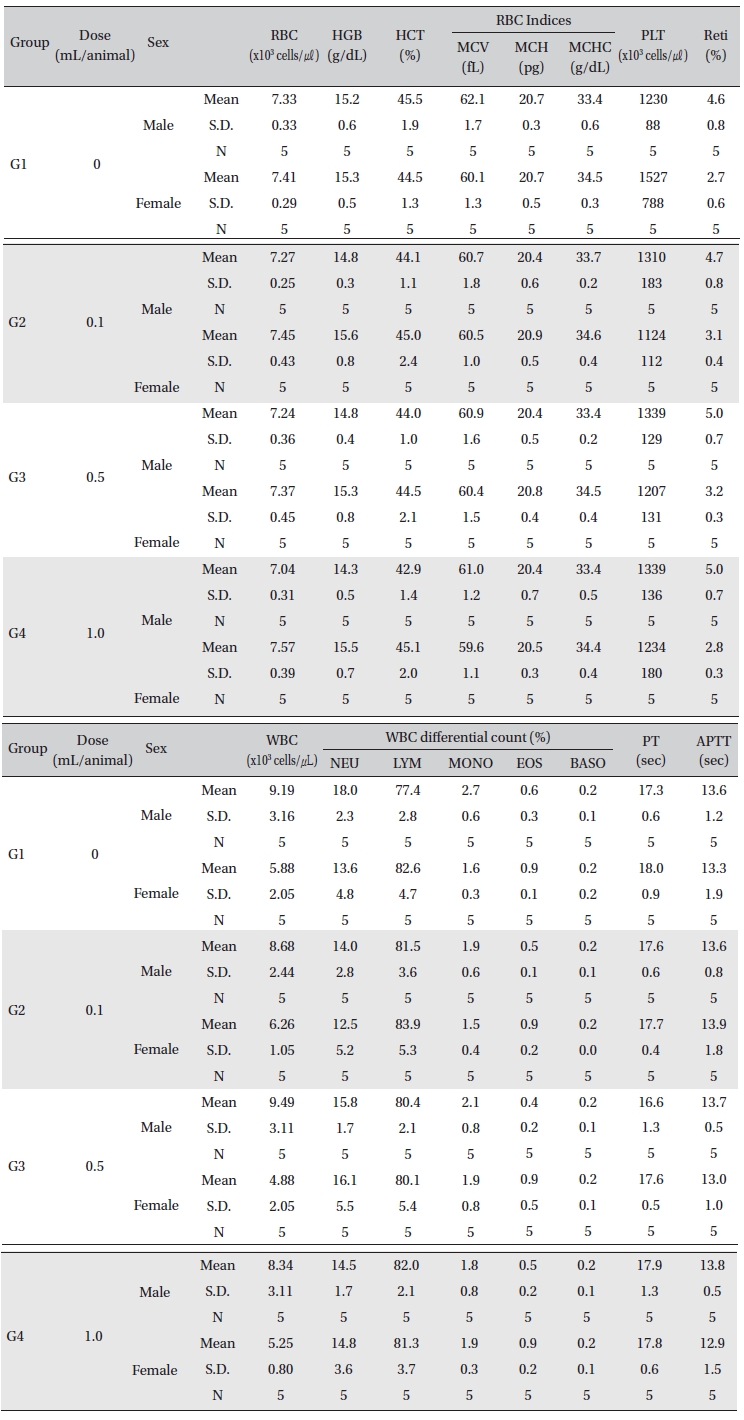
Mean hematology parameters
[Table. 6] Mean clinical chemistry
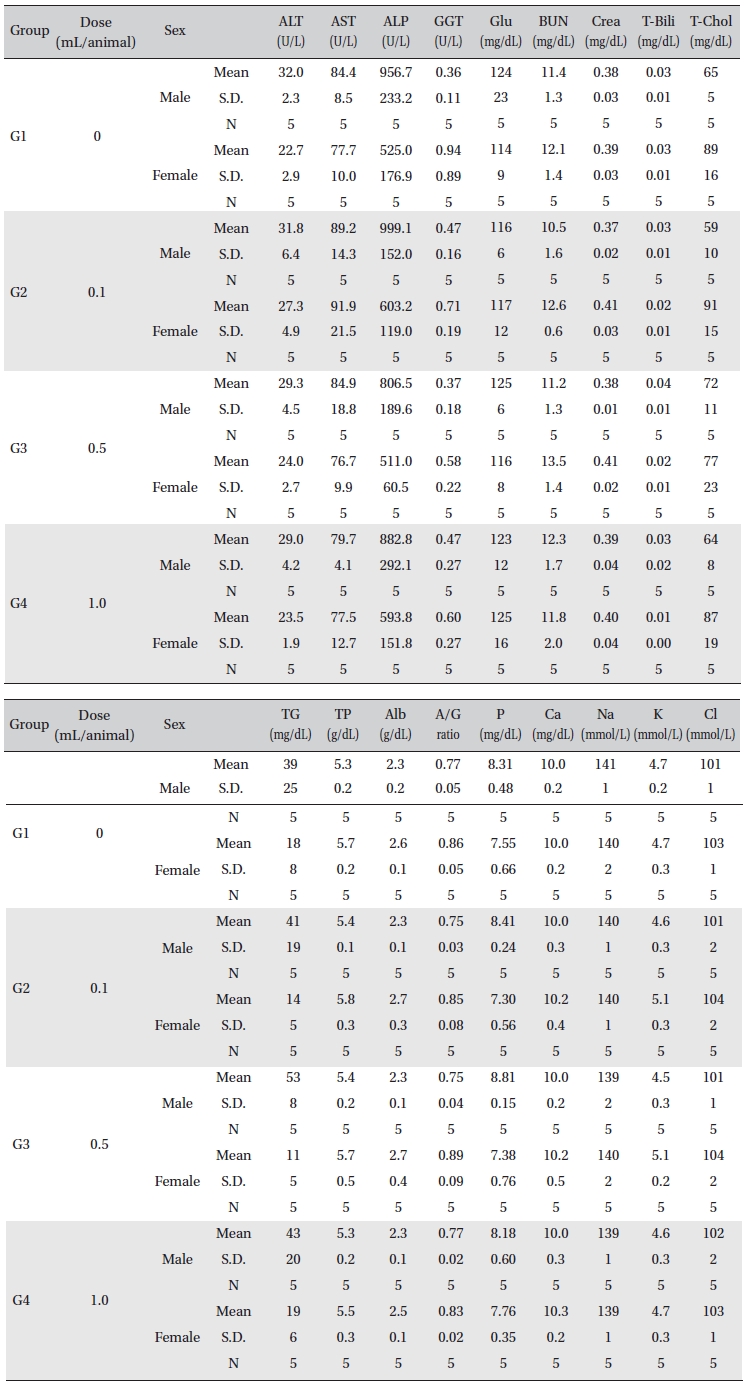
Mean clinical chemistry
[Table. 7] Mean clinical chemistry
Mean clinical chemistry
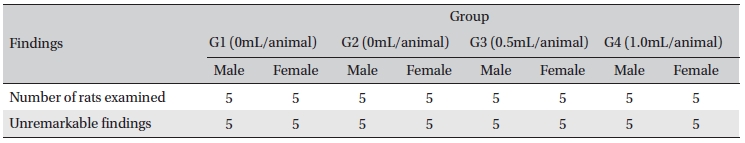
[Table. 8] Histopathological findings
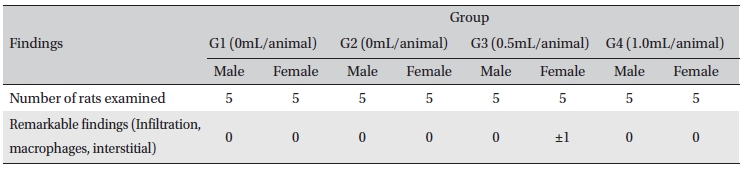
Histopathological findings
This study was performed to provide objective safety data for Chukyu pharmacopuncture. Doses of 0.1, 0.5, 1.0 mL of Chukyu pharmacopuncture were administered to the experimental groups, and a 1.0-mL dose of normal saline solution were administered to the control group. In all four groups, no deaths occurred, and no abnormalities were found. No significant changes in the clinical signs, weights, hematologic examination results and blood chemical test results were noted between the control group and the experimental groups. In necropsy for checking for abnormalities in organs and tissue, no significant histopathological findings were noted except for one case where interstitial infiltrating macrophages were found in one female rat in the 0.5-mL/animal group.
To assess the toxicity of Chukyu pharmacopuncture, we need to study its acute and chronic side effects and its relations with capacity reaction more. Animal testing is the most fundamental and basic way to perform safety assessments [22]. The Korea Food & Drug Administration has testing protocol guidelines for the study of toxicity, and all experiments should be conducted following Good Laboratory Practice (GLP) regulations [23]. In this study, a 1.0-mL dose of Chukyu pharmacopuncture caused no considerable side effects in either male or female rats, which indicates that this dose is safe to use and does not cause severe histological abnormalities. Further studies on the subject should be conducted to yield more concrete evidence to support this finding.
The results showed that administration of 1.0-mL/animal Chukyu pharmacopuncture did not cause any changes in weight or in the results of hematological, blood chemical, and necropsy examinations. It also did not result in any mortality, which indicates that Chukyu pharmacopuncture administration can be used as a safe treatment.